Typhoid in Bangladesh: A persistent public health challenge
One moment you’re minding your business, eating fuchka with suspiciously enthusiastic green water, the next you’re in bed negotiating with your thermometer and questioning every glass of tap water you have ever trusted. In Bangladesh, typhoid has become less of a disease and more of a character. That one relative who comes ‘for a night’ and then lives with you for six months, uninvited guests at weddings, exams and board results day, showing up precisely when your life was finally going well. It thrived in an era where pipes leaked and sanitation was more a suggestion than a system and boiling water was considered an optional lifestyle choice. Over time typhoid embedded itself into our collective memory, earning a reputation not just as a bacterial infection but as proof that you at some point had believed too much in roadside juice and too little in bacteria.
Typhoid fever has long been a silent but serious threat in Bangladesh. It affects tens of thousands of children and adults every year. Despite progress in public health, Bangladesh remains endemic for this bacterial infection driven by deep rooted challenges in water safety, sanitation, hygiene and emerging antimicrobial resistance. With the launch of one of the world’s largest typhoid vaccination campaigns in 2025, the country stands at a pivotal moment in its fight against typhoid. But understanding where the disease comes from, why it persists and what must be done requires a deeper look at its history in the context of public health.
So, what is typhoid?
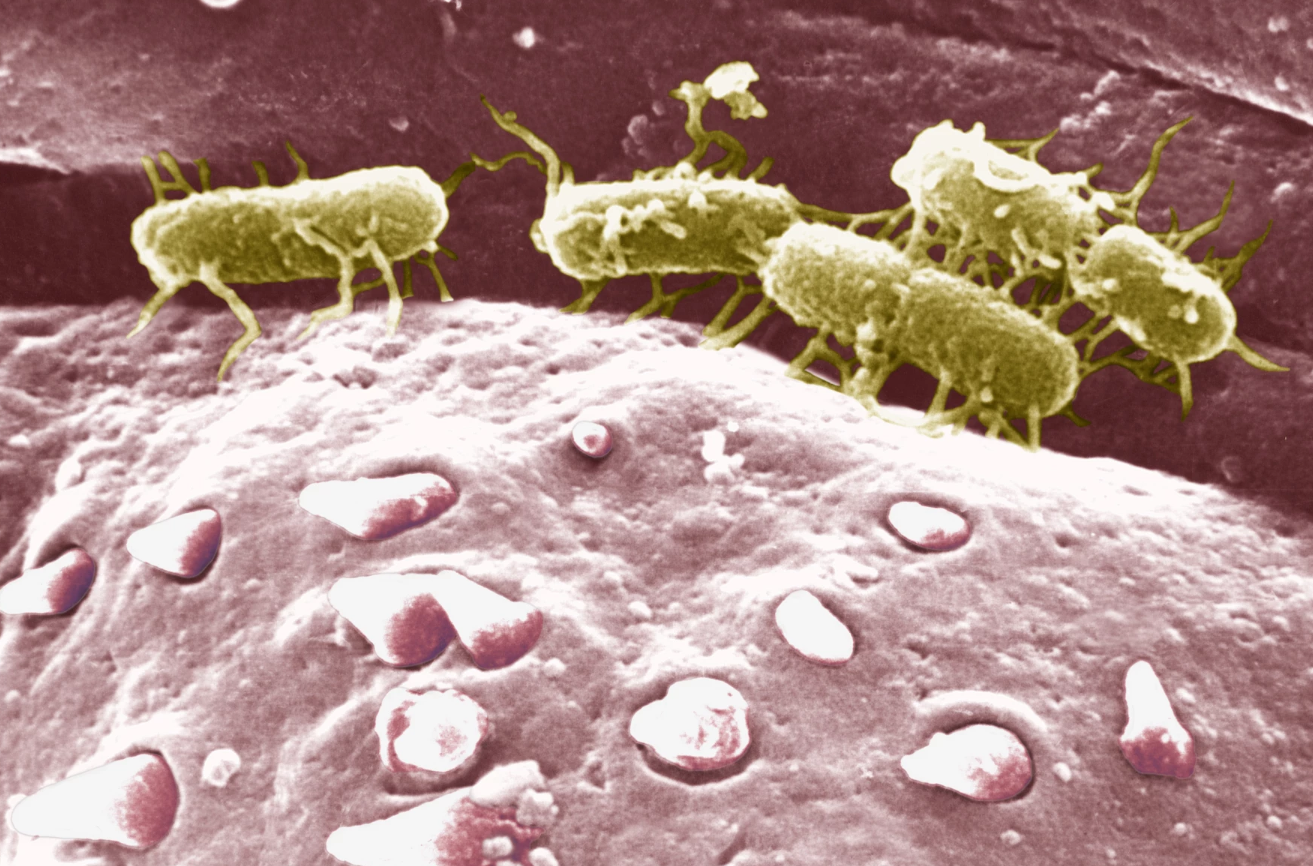
Typhoid fever is an acute bacterial infection caused by Salmonella enterica serovar Typhi. This is a gram negative bacterium with absolutely no manners and an unfortunate talent for thriving in places where sanitation is poor and clean water is more of an aspiration than reality. It does not need animals or insects to spread. Instead, it takes the low effort route by travelling through food or water contaminated with feces. This basically means someone, somewhere didn’t wash their hands and now you are paying the price.
Once inside the body, S. Typhi treats its new premium real estate with remarkable disrespect. Signaling its arrival with a high fever, weakness, stomach pain, headaches and a sudden tragic loss of appetite for foods you once could not stop eating. If left untreated, the situation escalates fast as typhoid can cause intestinal bleeding, bowel perforation and even death. This serves as a grim reminder that something microscopic can still completely derail and potentially end your life.
Typhoid in Bangladesh: Endemic status and burden
In Bangladesh, typhoid is an everyday reality not just a seasonal curiosity. In the crowded quarters of cities like Dhaka, the disease stays endemic as it circulates year round with pronounced peaks during and after the monsoon rains or when heavy rainfall, rising river levels and overwhelmed water systems push contaminated water into places it should never go. Research on typhoid in the Dhaka metropolitan area found that nearly half of all cases occurring during the monsoon months have clear links between rainfall patterns and increased infection rates. This seasonal surge reflects how waterborne pathogens like Salmonella Typhi exploit soggy conditions by turning streets, drains and shallow water sources into highways for disease transmission.
In the narrow lanes of settlements like Kamalapur, families share walls and water points and municipal infrastructure struggles under the weight of the city’s growth. In these environments, typhoid does not spread evenly but it follows the lines of inequality. Access to safe water and sanitation is not uniform and the difference between ‘sick’ and ‘well’ often comes down to a few simple but critical resources.
One of the most striking findings from studies in Kamalapur is that using a proper latrine for defecation is not just a matter of dignity. It is strongly protective against typhoid. When families had access to and consistently used latrines, they were far less likely to contract typhoid than their neighbours who did not. This is because latrines help keep human waste and the Salmonella bacteria within it and out of the fragile water supplies and food chains that already strain under the pressure of dense settlement and monsoon flooding.
To put it simply, in places where toilets are shared, improvised or absent, human excrement can end up mingling with the very things people drink and eat. In contrast, a properly built and used latrine breaks the cycle of contamination by keeping S. Typhi from hitching a ride from feces into someone’s mouth. For residents of urban slums that barrier as basic as a seat and a hole in the ground can mean the difference between weeks spent in hospital and weeks spent at work or school.
But the story of typhoid in Bangladesh isn’t just about one neighbourhood or one infrastructure gap. It highlights a broader truth about urban inequality. When water systems are poorly maintained, when drainage fails during monsoon downpours and when people lack basic sanitation, disease will obviously find room to thrive. Those who live in wealthier parts of the city can rely on boreholes, bottled water and private toilets. These are luxuries for many in informal settlements where broken pipes and open drains are part of daily life.
In a country where children and adults alike face this disease each year, the solutions are both structural and human. Improving sanitation, starting with widespread access to safe latrines and ensuring that every household has reliable, clean water are not just public health goals. They are lifelines in the truest sense. As Bangladesh tackles typhoid through vaccination campaigns and water sanitation programmes, the voices of those most affected families trying to keep their children safe during monsoon floods, parents weighing the cost of boiled water against daily expenses truly remind us that health equity is inseparable from human dignity.
Antibiotic resistance: A rising threat
One of the most alarming challenges in Bangladesh is the rise of antibiotic resistant typhoid strains. This is a concerning signal that the bacteria are evolving under antibiotic pressure. These resistant strains complicate treatment, increase costs and raise the risk of complications and mortality. The rise of resistance underscores the need for antibiotic stewardship (careful use of antibiotics) and stronger surveillance systems to track emerging bacterial patterns.
Antibiotic resistant typhoid is basically what happens when the typhoid bacteria get tired of being bullied by medicines and decide to fight back. In Bangladesh, this is becoming a serious problem. For years, antibiotics have been overused, misused, shared between family members or stopped halfway without finishing the course.This gives the bacteria just enough practice to learn how to survive. As a result, many typhoid infections no longer respond to common antibiotics. Meaning doctors are forced to use stronger, costlier drugs and patients stay sick for longer. This matters because when antibiotics stop working, even a ‘simple’ fever can turn dangerous, especially for children. The solution is not complicated but it does require awareness and health literacy. People need to know that antibiotics are not painkillers, not cures for every fever and definitely not sweets to be shared. Finishing the full prescribed dose, avoiding self medication as antibiotics only work for bacterial infection and not viral ones, trusting proper diagnosis can slow resistance. At the same time, vaccination against typhoid reduces the need for antibiotics altogether which means bacteria get fewer chances to evolve. In short, antibiotic resistance thrives on confusion and misuse but with better education, smarter medicine use and public awareness campaigns, Bangladesh can stop typhoid bacteria from becoming stronger than the drugs meant to defeat them.
Vaccination: A game-changer
In a landmark public health initiative, Bangladesh launched a nationwide Typhoid Conjugate Vaccine (TCV) campaign in October 2025. With support from WHO, UNICEF, Gavi (the Vaccine Alliance), and other partners, the government aimed to vaccinate approximately 50 million children aged 9 months to under 15 years.
Bangladesh became the eighth country in the world to introduce TCV at such a scale, reflecting its commitment to controlling a disease that remains a leading cause of febrile illness in children. The Expanded Programme on Immunization (EPI) strives for high coverage (95% or more) to generate strong population immunity and sharply reduce typhoid cases and deaths.

Bangladesh has also targeted high risk communities. The nationwide campaign also included targeted vaccination of nearly half a million Rohingya children in Cox’s Bazar camps where overcrowding, limited sanitation and unsafe water make outbreaks particularly likely.
Studies from Bangladesh and elsewhere show that typhoid conjugate vaccines significantly reduce disease incidence especially when combined with improvements in water, sanitation and hygiene at the household and community levels.
Beyond vaccines: Comprehensive public health strategies
While vaccination represents a major breakthrough in the fight against typhoid as it cannot stand alone. The disease is deeply rooted in structural and social conditions, meaning long term control depends on addressing the environments in which Salmonella Typhi continues to thrive. Safe water, adequate sanitation, informed communities and strong disease surveillance together form the backbone of a truly effective public health response.
At the heart of typhoid transmission lies unsafe water. Ensuring access to clean, chlorinated and reliably maintained water systems is one of the most powerful tools for breaking the fecal to oral transmission cycle. In Bangladesh, agencies such as the Department of Public Health Engineering are responsible for expanding and maintaining water and sewage infrastructure, yet aging systems, leaks and contamination remain ongoing challenges. Without continuous investment, monitoring and accountability, water meant to protect communities can easily become a source of infection.
Sanitation and hygiene are equally critical. The use of improved latrines, safe waste disposal and basic household water treatment methods such as boiling, filtering or chlorinating drinking water can significantly reduce exposure to typhoid bacteria. These practices do more than curb typhoid alone as they also reduce the overall burden of water borne illnesses that disproportionately affect children and low income households. However, the effectiveness of these measures depends on consistent use which is often shaped by access, affordability and public awareness.
Health education plays a powerful but sometimes underestimated role in prevention. Public awareness around safe food handling, regular handwashing with soap and the importance of completing vaccination schedules can empower families to take control of their own health. When communities understand how typhoid spreads and how easily it can be prevented through everyday practices prevention becomes a shared responsibility rather than a distant policy goal.
Behind the scenes, surveillance and research remain essential to guiding action. Institutions such as the National Institute of Preventive and Social Medicine and other research centers monitor disease trends, track outbreaks and study emerging antibiotic resistance. This evidence informs national treatment guidelines and helps policymakers respond to shifting patterns of infection before they escalate into larger public health crises.
Despite measurable progress significant challenges persist. Gaps in water and sanitation infrastructure continue to allow typhoid to circulate particularly in underserved urban and peri urban areas. The rise of antimicrobial resistance threatens to make treatment more complex and expensive, demanding careful antibiotic stewardship and ongoing research into alternative therapies. Rapid urbanization especially in cities like Dhaka places immense strain on already fragile systems. This increases the risk of contamination. At the household level socioeconomic barriers often prevent consistent adoption of safe water and sanitation practices. This underscores that typhoid is not just a medical issue but a reflection of inequality itself.
A path to typhoid control
Typhoid fever in Bangladesh is more than a clinical diagnosis. It is a marker of deeper public health challenges tied to water, sanitation, social inequities and microbial evolution. Bangladesh’s nationwide vaccination campaign is a bold step that signals renewed commitment to child health and disease prevention. Combined with improvements in water quality, sanitation, hygiene and antibiotic stewardship, the country can dramatically reduce the burden of typhoid and protect future generations.
For policymakers, healthcare providers and communities alike, the fight against typhoid must be holistic, sustained, rooted in both scientific evidence and grassroots action. Only then can Bangladesh move closer to a future where typhoid is no longer a persistent threat.
Maisha Quadery is an A-level student and an aspiring public health advocate. Reach her at maishaquaderyhumaira@gmail.com
Send your articles for Slow Reads to slowreads@thedailystar.net. Check out our submission guidelines for details.



