How poor governance broke Bangladesh's immunisation model
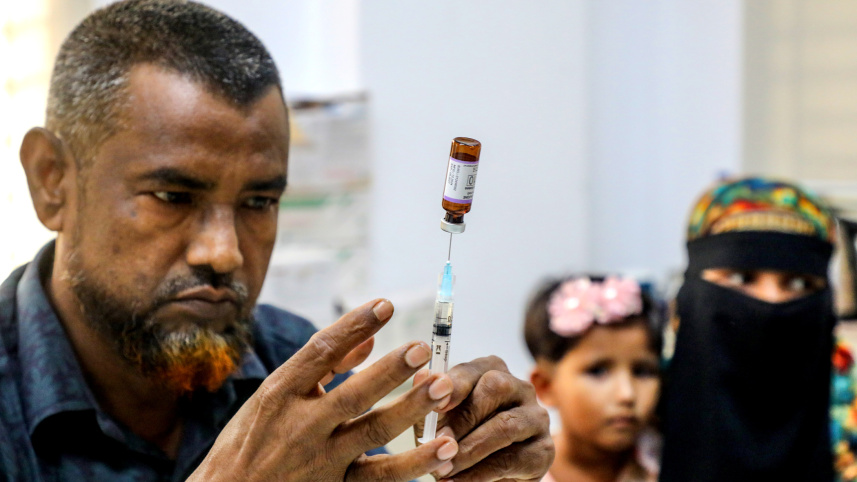
Bangladesh’s Expanded Programme on Immunization (EPI) has long been one of the country’s most celebrated public health successes. Built on sustained government commitment, strong development partnerships, and a vast network of frontline health workers, it delivered consistently high coverage and sharply reduced the incidence of vaccine-preventable diseases. For years, it positioned the country as a model for the developing world.
That model is now being undone. The ongoing measles vaccine crisis is not merely an isolated disruption but points to institutional weakening. National vaccination coverage reportedly fell to around 60 percent in 2025, the lowest in nearly a decade, down from 85-92 percent between 2010 and 2022.
Such steep declines do not occur suddenly or without warning. It is not merely due to a logistical problem. It is a failure of governance. Immunisation systems depend on predictable structures: coordinated procurement, stable financing, functioning leadership, and a reliable workforce. When these are disrupted—especially simultaneously—the system breaks down.
For years, vaccine procurement operated under the Health, Population and Nutrition Sector Programme (HPNSP), which provided a clear and functional administrative pathway. Its effective dismantling in 2025, without a credible transition mechanism, represents a critical policy failure. There is little evidence that this decision was guided by broad technical consultation or risk assessment, an omission that is difficult to justify given the stakes.
The consequences were foreseeable: delayed approvals, leadership gaps, and uncertainty in funding flows. These are direct outcomes of institutional disruption and cannot be written off as technical glitches. At the same time, the system failed to confront a growing and highly visible threat: misinformation. Vaccine hesitancy did not emerge overnight either. It intensified during the Covid pandemic and continued to spread, largely unchecked. What was needed was sustained public communication and active counter-engagement. What followed instead was a deafening silence.
The impact became evident during the 2025 Typhoid Conjugate Vaccine campaign, where misinformation drove refusal rates high enough to push coverage below herd immunity thresholds in several urban areas. Misinformation does not need active advocates so much as it thrives in the absence of challengers or counterarguments. Equally concerning is the lack of urgency around emerging scientific questions. Why are infants under six months increasingly vulnerable? Are maternal antibodies weakening? Is the virus evolving? These are not just academic concerns; they are central to programme strategy. Yet, they remain insufficiently investigated, reflecting a deeper neglect of research and evidence-based planning.
The system’s structural weaknesses are equally stark. Nearly 45 percent of EPI field-level positions in 37 districts remain vacant. These workers operate across roughly 150,000 vaccination centres, which are the backbone of the immunisation programme. Without them, coverage declines are inevitable. Meanwhile, vaccine porters responsible for maintaining the cold chain reportedly went unpaid for months, triggering unrest and nationwide strikes. A system that cannot sustain its frontline workforce cannot sustain its outcomes.
Data systems tell a similarly incomplete story. Despite reassuring “official” coverage figures, a 2025 joint analysis by Unicef, WHO, and Gavi suggests that hundreds of thousands of children remain under-immunised, particularly in urban areas. The gap is not just in delivery but also in visibility. Fragmented data systems that exclude private and informal providers create blind spots, preventing timely intervention.
This pattern is not confined to immunisation. A parallel regression is underway in family planning—another sector once considered a global success. Bangladesh reduced its total fertility rate from 6.3 in 1975 to 2.3 by 2022. That progress is now reversing, with the rate rising to 2.4. As per a recent report citing data from the Directorate General of Family Planning (DGFP), more than one-third of the 487 upazilas in the country have run out of all types of government-supplied contraceptives. Condoms are out of stock in 397 upazilas, while at least 220 upazilas have run out of oral pills. Meanwhile, implants, intrauterine devices (IUDs), and injectables are out of stock in all upazilas.
The causes are familiar: workforce shortage, procurement breakdown, and weakening institutional structure. Nearly 28 percent of sanctioned posts within the Directorate General of Family Planning (DGFP), from the central to the field level, remain vacant, according to another report.
What these trends expose is a deeper vulnerability: the inability to protect essential public health systems from administrative disruption. Dismantling functioning systems without tested alternatives is far from reform. Such steps only scale up the risk to a national level. And we are now paying that price.
The priority now must be to restore institutional stability, re-establish clear procurement pathways, urgently fill workforce gaps, invest in research and surveillance, and rebuild public trust through sustained communication. Just as importantly, critical health systems must be insulated from abrupt policy shifts and administrative discontinuity. If addressed now, the broader system stress remains manageable. If not, they will escalate into crises that are far more costly, both financially and in human terms.
The narrative of success that once defined Bangladesh’s health sector was built over decades. It is now at risk of being undone in a matter of years. Unless there is a course correction, this will not be remembered as a temporary setback, but as a preventable reversal.
Zahida Fizza Kabir is a social entrepreneur and CEO at SAJIDA Foundation.
Views expressed in this article are the author's own.
Follow The Daily Star Opinion on Facebook for the latest opinions, commentaries, and analyses by experts and professionals. To contribute your article or letter to The Daily Star Opinion, see our guidelines for submission.



 For all latest news, follow The Daily Star's Google News channel.
For all latest news, follow The Daily Star's Google News channel.
Comments