Precision over power: How proton therapy is transforming cancer care
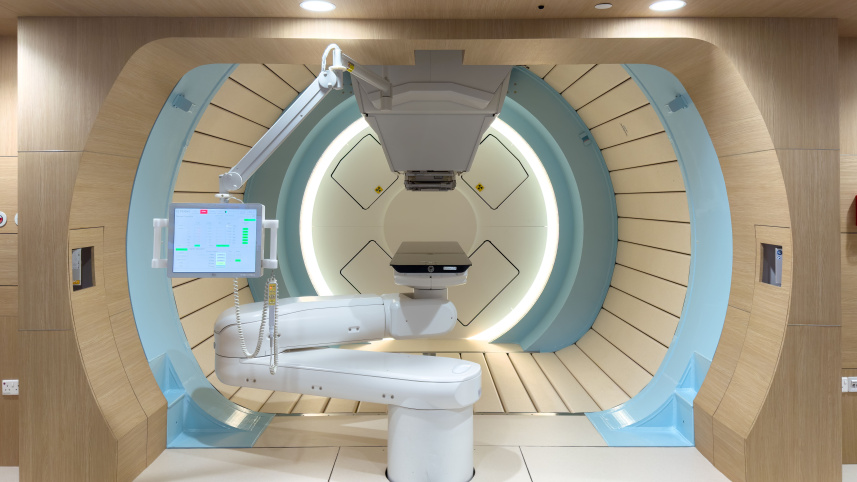
Cancer treatment has long relied on a delicate balance—destroying tumours while sparing the healthy tissues that sustain life. In recent years, that balance has begun to shift, thanks to advances in radiation technology. At the forefront of this transformation is proton beam therapy, a highly precise form of radiotherapy now being used at the National Cancer Centre Singapore (NCCS).
For Clin Asst Prof Kiattisa Sommat, Senior Consultant in Radiation Oncology, this technology represents not just innovation, but a meaningful change in how patients experience cancer treatment.
At the newly established Goh Cheng Liang Proton Therapy Centre at the NCCS, doctors are using cutting-edge radiation techniques such as proton therapy to target tumours more precisely while protecting healthy tissues. In this interview, she explains how modern radiotherapy is transforming cancer care and what patients should know about these advances.
How radiation fights cancer
Radiation therapy remains one of the three main pillars of cancer treatment, alongside surgery and chemotherapy. It is widely used, with more than half of cancer patients receiving it at some stage—either to cure the disease or to relieve symptoms such as pain.
The principle is straightforward but powerful. High-energy radiation is directed at cancer cells, damaging their DNA. Unlike normal cells, cancer cells have a reduced ability to repair this damage. As a result, they stop multiplying and eventually die.
Yet conventional radiation, which relies on X-rays, has a limitation: while it can target tumours effectively, it also exposes surrounding healthy tissues to radiation as the beam passes through the body.

What makes proton therapy different
Proton therapy takes a markedly different approach. Instead of X-rays, it uses positively charged particles—protons—that can be controlled with far greater precision.
What makes protons unique is their ability to deposit most of their energy at a specific depth and then stop. This means doctors can deliver radiation directly to the tumour while minimising exposure to tissues beyond it.
In practical terms, the difference is significant. Where conventional radiation may affect tissues both before and after the tumour, proton therapy can reduce what clinicians call the “exit dose”—the radiation that continues past the target. The result is a more focused treatment that better preserves healthy organs.
Fewer side effects, better quality of life
This precision translates into tangible benefits for patients. One of the most important is a reduction in side effects.
For patients with head and neck cancers, for instance, radiation can affect critical structures involved in swallowing, taste, and saliva production. Proton therapy allows doctors to spare these areas more effectively. Patients are therefore more likely to maintain their ability to eat, speak, and carry out daily activities during and after treatment.
Over the long term, this approach may also reduce the risk of secondary cancers—an important consideration, particularly for younger patients.
A vital option for children with complex cancers
While proton therapy is not a universal solution, it is especially valuable for certain patient groups.
Children stand to benefit the most. Because their bodies are still developing, they are more vulnerable to the long-term effects of radiation. Exposure to healthy brain or body tissues can lead to complications such as learning difficulties, growth problems, or secondary cancers decades later. By limiting unnecessary radiation, proton therapy helps protect their future health.
The technology is also particularly useful for tumours located in difficult or sensitive areas—such as the brain, spine, or near vital organs—where precision is critical.
Not for everyone
Despite its advantages, proton therapy is not suitable for all cancer patients. Decisions are made carefully, based on multiple factors.
The type and stage of cancer are central considerations. If the disease has already spread widely, local treatments like proton therapy may offer limited benefit. Patient-related factors also play a role. Because the treatment requires high accuracy, patients must remain still during each session. Even small movements can affect the delivery of radiation.
Technical factors, such as implants or anatomical variations, may also influence whether the therapy can be delivered safely and effectively.
And then there is cost. Proton therapy is significantly more expensive—often two to three times the cost of conventional radiotherapy. As a result, it is typically reserved for cases where its benefits clearly outweigh those of standard treatment.
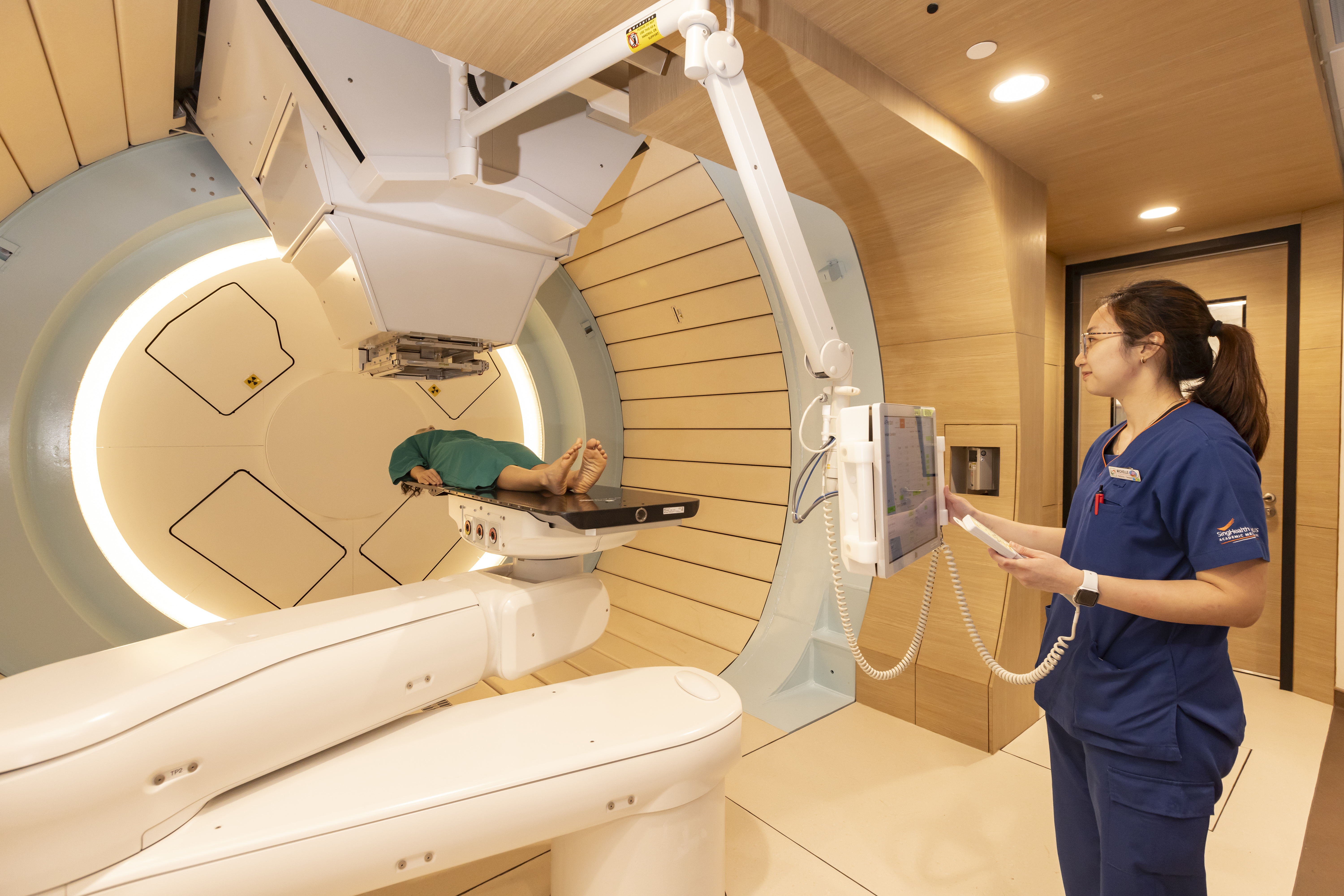
Inside the treatment process
Behind the scenes, proton therapy is one of the most meticulously planned treatments in modern medicine.
The process begins with consultation and detailed imaging, followed by a complex planning phase that can take around two weeks. During this time, specialists map out the exact dose and trajectory of radiation.
Treatment itself is usually delivered on an outpatient basis. Patients attend sessions five days a week, with each session lasting between 20 and 45 minutes. Depending on the cancer type and stage, the full course may last anywhere from one to seven weeks.
A multidisciplinary team—including radiation oncologists, medical physicists, therapists, and nurses—works together to ensure both precision and patient support throughout the process.
A growing global presence
Proton therapy is gaining traction worldwide, with more than 100 centres currently in operation. Singapore has emerged as a regional leader, with three centres offering the treatment.
At NCCS, the Goh Cheng Liang Proton Therapy Centre began treating patients in 2023. Within a few years, it has already managed hundreds of cases across a wide age range—from very young children to elderly patients—reflecting both the versatility and growing demand for the technology.
Looking ahead
For Dr Kiattisa Sommat, the promise of proton therapy lies not only in its technical sophistication but in its potential to redefine patient care.
Cancer treatment is no longer just about survival. Increasingly, it is about how patients live during and after treatment—how well they can eat, speak, think, and function in everyday life.
Proton therapy is one step towards that goal. It may not replace conventional radiotherapy, but for selected patients, it offers a more refined, targeted, and patient-centred approach.
As technology continues to advance, the future of cancer care may well be defined not by how aggressively we treat disease, but by how precisely we do so.



 For all latest news, follow The Daily Star's Google News channel.
For all latest news, follow The Daily Star's Google News channel.
Comments