Will we learn any lesson from the measles deaths?
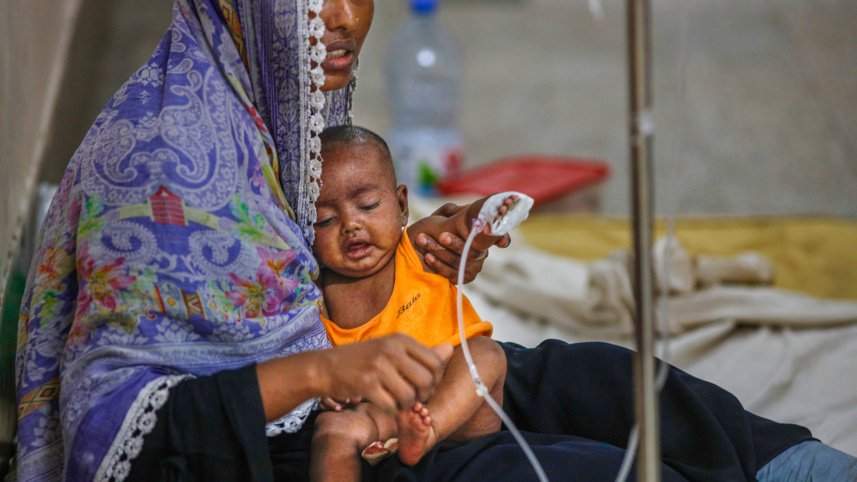
Every report of a child dying from the ongoing measles outbreak has left us not only saddened, but ashamed. Measles is not an unknown disease; medical science has long discovered how it spreads, the risks it carries, and how it can be prevented. So when children still die from measles, it is not simply because of the disease but also a clear sign of an inadequate public health system, failure in policymaking, and a lack of national priority. These deaths were not unavoidable. With timely vaccination, proper surveillance, early detection, and effective public awareness, many of them might have been prevented.
This is where the lessons of the Covid pandemic should return with renewed force. Covid taught us that health is not an isolated sector—it is the foundation on which all other sectors depend. When a public health system falters, the economy slows, schools close, jobs become uncertain, social stability weakens, and even national security comes under pressure. Many countries recognised this quickly and acted accordingly. They understood a simple truth: the end of a pandemic does not mean the end of risk. It means the work of preparing for the next crisis must begin immediately.
Unfortunately, in Bangladesh, we did not absorb that lesson with the seriousness it deserved. The recent measles deaths represent a stark reminder that we still remain largely reactive in handling public health crises. We hold meetings after disease spreads, issue statements after lives are lost, and become active only when the issue gains public attention. But we have not made timely and consistent immunisation, early risk detection, stronger field-level capacity, better data systems, and active emergency preparedness a regular part of health governance.
For this reason, measles deaths should not be viewed as an isolated crisis. They warn us of a much larger reality: our public health system remains fragile, preparedness is incomplete, coordination is weak, and long-term thinking is inadequate. Unless we build a comprehensive biosecurity system, including domestic vaccine production, we may face more loss of life in the future, whether from another pandemic, worsening endemic diseases, or sudden outbreaks.
In fact, treating health crises as temporary events remains to be a persistent error in judgement on our part. We tend to believe that once one wave passes, the danger has passed with it. But public health does not work that way. Threats are layered and continuous. Sometimes, they come as a new virus, sometimes as the return of an old infection, a climate-related disease spread, antimicrobial resistance, or a rapid transmission driven by urban crowding and poverty. That is why a health system must be prepared not only to treat patients, but also to anticipate risks, respond quickly, make evidence-based decisions, and maintain public trust.
The case of vaccine production makes the weakness in our public health system even more visible. The state-run Essential Drugs Company Ltd’s (EDCL) vaccine production project remains stuck in the land acquisition stage. After the government approved the project in 2023, land was initially acquired in Gopalganj. But in 2025, under the interim government, it was decided that the project would instead be implemented in Munshiganj’s Sirajdikhan. Meanwhile, there is still no meaningful effort to build the skilled workforce needed for such a highly technical project. At this point, it is urgent to create an appropriate organogram, recruit the necessary personnel, and place them under proper training both at home and abroad. At the same time, technology transfer must be secured through agreements with experienced vaccine manufacturers around the world. This issue deserves the urgent attention of the highest levels of government.
Public health is a political commitment. If primary healthcare, immunisation, disease prevention, surveillance, laboratory capacity, emergency preparedness, local health workers, supply systems, and data-driven decision-making are not prioritised, then no crisis is truly unexpected. The ongoing measles situation reflects exactly that condition of unpreparedness. Post-Covid health reform was needed not only on paper, but in practice, and it is still needed now. This is not just about one disease, but the entire system.
The measure of a civilised society is not found just in development statistics. It is also found in the protection it offers to its most vulnerable people. If we cannot protect the lives of children, then our story of development remains incomplete. And if even a warning as serious as measles does not awaken us, the price we pay in the next major health crisis may be even greater. Covid taught us one essential truth: health must come first, everything else follows. The measles outbreak is now teaching us another: if we don’t want to lose our children to preventable deaths, ensuring vaccination for every child must be our first priority. And for that, we must build a comprehensive biosecurity system, including vaccine production.
The question now is whether we will turn these lessons into policy, institutions, and action, or continue to nurture a culture of inaction and prepare, once again, only for mourning the next public health crisis.
Dr Syed Abdul Hamid is professor in the Institute of Health Economics at the University of Dhaka and convener at the Alliance for Health Reforms Bangladesh.
Views expressed in this article are the author's own.
Follow The Daily Star Opinion on Facebook for the latest opinions, commentaries, and analyses by experts and professionals. To contribute your article or letter to The Daily Star Opinion, see our guidelines for submission.




 For all latest news, follow The Daily Star's Google News channel.
For all latest news, follow The Daily Star's Google News channel.
Comments